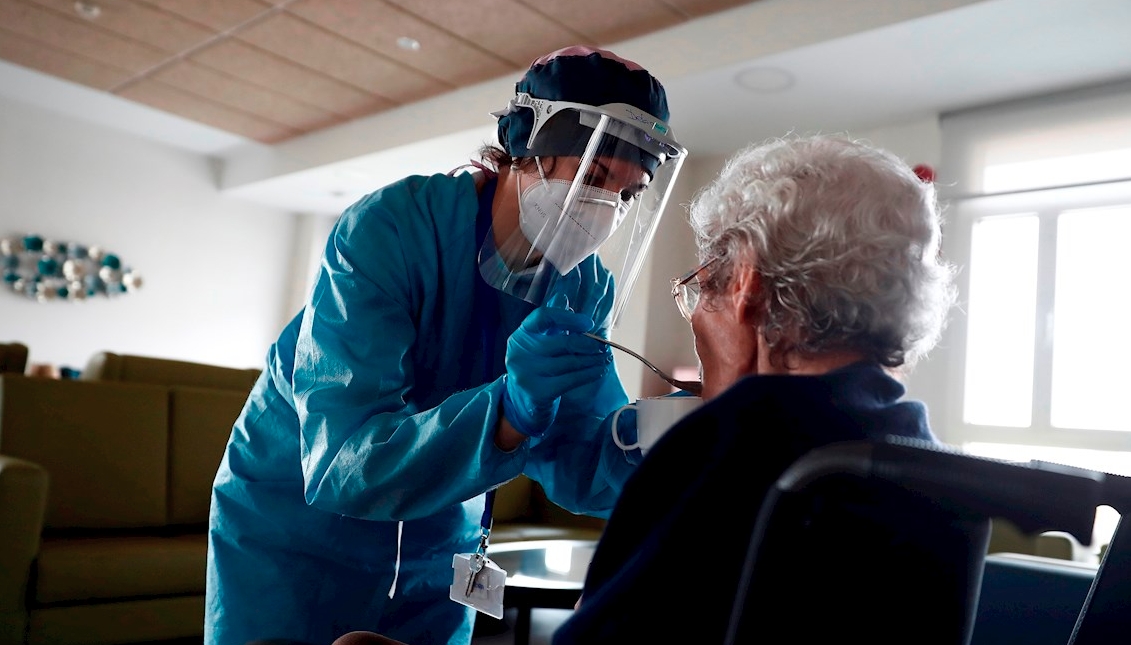
New report decries a "human rights violation" in nursing homes during the COVID-19 pandemic
According to a new document published by Amnesty International, during the first wave of COVID-19, human rights violations of the elderly were rampant in…
Domingo has not seen his granddaughter for months. Not that he saw her much earlier, Sunday mornings at best. But since the coronavirus pandemic hit and paranoia spread, he no longer distinguishes between weeks. It took half a year of doubt and uncertainty before they could meet again, so he could see how much she had grown.
But loneliness and closure were not the greatest perils, just the most emotional. It is worse to walk through his residence and realize more than half the staff is missing, that there are not enough nurses to attend to them in the morning and a lack of assistants to manage meals and medications. All of this is in the midst of a global health crisis stirred on by the media's hysteria.
The reality is that there have been many problems and institutional shortcomings in the societal relationship with senior citizens. If they were already terrible, it has only been worsened by the pandemic and the poor management of nursing homes. In countries where quarantine measures are not in place, the situation is much more extreme as citizens and facilities are not aware of the risk to patients. An ageist population and policies only generate the same kind of risk.
RELATED CONTENT
All of this was partially reflected in a recent report by Amnesty International Spain, which warns that, especially in Madrid and Catalonia, at least five basic human rights were violated in nursing homes: the right to health with austere measures that reduced personnel and resources, the right to life and non-discrimination when orders were given not to transfer certain patients to avoid overwhelming the ICUs, the right to private and family life hindered by more extreme confinement than the rest of society under lockdown, and the right to a dignified death.
The report notes certain improvements in the second wave of the COVID-19, but above all, it warns of the impoverishment of the medical profession, which had a major impact among all the working staff. Added to massive influx of COVID-19 patients, hospitals and health centers often operated with more than half their staffs on leave in March and April.
It also emphasizes that depending on the class of the patients, there were people who faced discrimination and had less access to treatment at the height of the virus' explostion. The lack of facilities in small cities is also something officials are rethinking as part of post-COVID health policies and an urgent review of the protocols for visits.










LEAVE A COMMENT:
Join the discussion! Leave a comment.